Are You turning 65 and have questions about medicare health insurance plans?
Let us help you navigate Medicare Plans in Oregon in 3 Steps.

STEP 1: Understand Original Medicare
A Zolezzi Insurance agent will answer your Medicare questions.
Step 2: explore your medicare options
There are several Medicare plans available in Oregon for you from.
step 3: choose your plan and enroll
We can help you choose the right plan and enroll when you are ready.

The right Medicare choices start here
- If you’re new to Medicare, you probably have lots of questions. What happens if you keep working past 65?
- Will Original Medicare be enough to pay for the high cost of health care? And what are your options?
We have answers. This page will help you understand the various Medicare choices available to you and help you make informed and confident decisions.
What Are the Things you should know about Medicare
Medicare is the nation’s largest health insurance program, with nearly 68 million beneficiaries. Yet, most people don’t know what Medicare covers or what it costs. TO GET STARTED, LET’S LOOK AT SOME THINGS YOU NEED TO KNOW:- Medicare does not cover all costs associated with your health care. It was never intended to cover all of your medical expenses.
- Medicare is not free. While most people do not pay a premium for Part A, there is a premium associated with Part B.
- Medicare is not simple. Medicare benefits are offered directly from the government or through private insurance plans. There are many things to consider when choosing Medicare benefits. Health care coverage is an important financial safety net to Americans age 65+ and those with disabilities.
- Choosing the right Medicare coverage is critical. A Zolezzi Insurance Agent is a reliable resource to help you every step of the way.
STEP 1: Understand Original Medicare
Original Medicare has two parts:
- Part A – Hospital Insurance
- Part B – Medical Insurance

Part A – Medicare Hospital Insurance
What it helps cover:
- Inpatient care in hospitals, including the room, nursing services, and supplies
- A stay in a skilled nursing facility (SNF)
- Home health and hospice care if they are medically necessary
What does it cover:
Before Medicare Part A benefits kick in, you are responsible for paying a deductible. Your deductible must be met each benefit period, which begins the day you’re admitted to a hospital or SNF. The benefit period ends when you haven’t received any hospital care or skilled care for 60 days in a row. If you are admitted to a hospital or SNF after one benefit period has ended, a new benefit period begins. You are also responsible for paying some of the costs after your deductible is met.
Your share of the Part A costs in 2021:
• $1,484 deductible for days 1 – 60 each benefit period
• $371 per day copay for days 61 – 90 of hospitalization
• $742 per day copay for days 91 – 150 of hospitalization
• $185.50 per day copay for days 21 – 100 of an (SNF) stay
What it costs:
There is no monthly premium for Part A as long as you or your spouse paid into Social Security for at least 10 years.

What does this mean to you?
Original Medicare is a beneficial program that helps ensure that the health care you need is covered. But you still could be left with thousands of dollars of out-of-pocket medical costs. Examples of your costs with Original Medicare: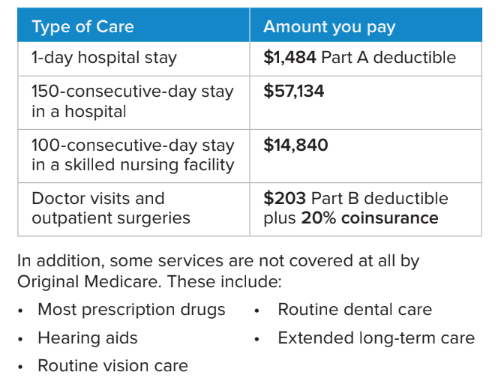
Part B – Medical Insurance
What it helps cover:
• Services doctors provide in their offices and in hospitals
• Services from other health care providers
• Outpatient care and home health care
• Durable medical equipment, like wheelchairs and walkers
What it doesn’t cover:
You must pay your annual deductible before Medicare Part B begins to pay benefits, and you must pay a share of the cost for services.
Your share of the Part B costs in 2021:
• $203 deductible
• 20% of the Medicare-approved amount for covered services
• There’s no yearly limit on your out-of-pocket costs
What it costs:
You pay a monthly premium, which in 2021 starts at $148.50 and increases on a sliding scale based on income. People with annual incomes over $88,000 will pay more. The premium is
usually taken out of your Social Security check.
What is the “Medicare-approved amount?”
Each year, the Centers for Medicare and Medicaid Services (CMS) lists the amounts it will cover for hospital and medical services. Most doctors accept these amounts and will charge you the Medicare-approved rate. If you use a doctor who charges more than the Medicare-approved rate, you will be responsible for paying the difference—up to 15% over the Medicare-approved rate—as well as the usual Medicare deductible and coinsurance costs
STEP 2: Explore Your Medicare Options
Because Original Medicare doesn’t cover everything, most people choose additional coverage to help protect themselves from high medical costs. Optional coverage is offered by private insurance companies that contract with the federal government.

Part C – Medicare Advantage Plans
How it works:
Medicare Advantage plans combine Medicare Part A and Part B coverage into one plan offered by a private insurance company, so you get all your hospital and medical benefits from one source. Most Medicare Advantage plans are either Health Maintenance Organization (HMO) plans or Preferred Provider Organization (PPO) plans.
What it covers:
You get all the benefits of Original Medicare, and most plans also include Part D prescription drug coverage. They may also cover extra days in the hospital; dental, vision, and hearing benefits; fitness program memberships; and other wellness benefits. Benefits, plan coverage areas, and provider networks can vary widely.
What it costs:
Monthly premiums vary by plan; most Medicare Advantage plans include Part D drug coverage as part of their monthly premium. You must enroll in Parts A and B and pay your Part B premium. You may have to pay a copay or coinsurance for some services, but you can typically save money by using a provider in the plan’s network.
What’s most important to you?
Savings and coordinated care.
- Your primary care physician coordinates your care
- Typically lower premiums
Affordable copays
Part D – Prescriptions Drug Coverage

How it works:
Medicare Part D covers prescription drug costs. You are eligible to enroll in Part D once you are entitled to Medicare Part A or enrolled in Part B. You can pair a stand-alone Part D plan with Original Medicare, or choose a Medicare Advantage plan (Part C) that includes Part D coverage.
What it covers:
Benefits will vary by plan. Each drug plan maintains a list of covered drugs (known as a formulary) and has their own unique rules and costs. Here are Medicare’s standard benefits in 2021:
- Some drug plans have a yearly deductible that resets every calendar year on Jan. 1. After the deductible, you usually pay a copay or coinsurance for each fill.
- If your prescription costs reach $4,130 during the year, you enter the coverage gap, or “donut hole,” and pay 25% coinsurance for each fill.
- You leave the coverage gap once your total out-of-pocket expenses reach $6,550. Then you pay a smaller portion of the cost and your Part D plan pays the rest until the end of the calendar year (Dec. 31).
What it costs:
Monthly premiums vary by plan, and your out-of-pocket costs will depend on the type and quantity of prescription drugs you take.
Think About…
If you don’t choose a Medicare Part D plan when you are eligible and don’t have other creditable drug coverage, there will be a penalty for every month you could have enrolled but didn’t. So it may pay to enroll even if you don’t use prescription drugs now.

How it works:
Medigap plans help “close the gaps” in Original Medicare by paying for many of the costs that Original Medicare doesn’t cover, like copays, coinsurance, and deductibles. There are no networks, so you have the freedom to choose your own providers as long as they accept Medicare.
What it covers:
You have a range of plans and benefits to choose from. Medigap plans are standardized by the government and are identified by the letters A through N.
- IMPORTANT: Medigap plans do not include prescription drug coverage.
- You can add a Part D prescription drug plan.
- For a comparison of standardized plans, go to Medicare.gov.
- Not all plans may be available in your area.
What it costs:
Monthly premiums can vary greatly depending on the plan you choose and the insurance company you buy from. Although monthly premiums for Medigap plans are usually higher than those for Medicare Advantage plans, you will typically have fewer out-of-pocket costs when receiving medical services under Medigap coverage.
Keep in mind…
No matter which insurance company you buy from, you’ll get the same basic benefits. Some companies also include extras such as a fitness club membership and discounts on health care products. So even though the basic benefits are standardized, plans aren’t all the same. When you compare plans, be sure to look at more than the price. Also, consider the value of any extra
benefits, as well as the company’s reputation and service.

STEP 3: Choose Your Plan and Enroll
Now that you’ve reviewed your Medicare benefits and options, you’re ready to dive in. Learn about the best times to enroll so you can avoid penalties and get the type of plan you want.

Your Initial Enrollment Period is a seven-month window—from three months before your birthday month to three months after your birthday month.
Initial Enrollment Period
If you plan to retire at 65, your Initial Enrollment Period (IEP)
begins three months before, and ends three months after, your 65th birthday month. Coverage can begin as soon as the first day of the month you turn 65.
IMPORTANT:
- You must already be enrolled in Original Medicare Parts A and B in order to enroll in a Medicare Advantage, Medigap, or Part D drug plan.
- Unless you have creditable drug coverage from an employer, union, VA, or other means, you must obtain Part D coverage during your IEP or you could incur a late enrollment penalty.
- If you already receive Social Security benefits, enrollment in Medicare Parts A and B is automatic.
- If you are under 65 and disabled, you will automatically be enrolled in Part A and Part B after your first 24 months of receiving disability benefits from the Social Security Administration.
- If you choose a Medigap plan, you should apply when you are first eligible, and coverage can begin the same day your Part B coverage starts. You are guaranteed acceptance within six months of your Part B effective date, regardless of any pre-existing conditions.
- If you enroll after six months, you could be subject to underwriting and may not qualify, or have to pay more, for the plan you want.
Annual Enrollment Period (AEP)—Oct. 15–Dec. 7
During this time you can apply for any type of Medicare plan—Parts A, B, C (Medicare Advantage), D (Prescription Drug), and Medigap. It is also the time when you can freely move between plan types (for example: from Original Medicare to a Medicare Advantage plan) or shop around for a plan that better fits your needs.
Open Enrollment Period (OEP)—Jan. 1–Mar. 31
This period is limited to those enrolled in a Medicare Advantage
plan. During this time you can switch from your current Medicare
Advantage plan to another Medicare Advantage plan (with or
without drug coverage) or to Original Medicare (with or without a
Part D drug plan).
IMPORTANT:
If you’re on Original Medicare or any other plan type, you cannot change plans during this time. You will need to wait for the Annual Enrollment Period or a Special Enrollment Period (if you qualify).
Special Enrollment Period (SEP)
Certain events may qualify you for a change in your Medicare coverage, such as leaving your plan’s service area or changes to your financial eligibility. The timing of your SEP depends on the circumstances that created the need to change plans. For example, if you qualify for Extra Help with Medicare drugs costs, you have three months from the notification date to change your Medicare Advantage or Part D drug plan. If you think you may qualify for a SEP, call us for more information.
Get a Quote




